“The use of simulation is not a one-off resource, but a strategic tool for improving patient care”
SJD Barcelona Children's Hospital integrated a high-fidelity SIMTest before administering, for the first time in Spain, a gene therapy for SPG50, strengthening team coordination and anticipating risks in an extremely complex procedure.

In September 2025, SJD Barcelona Children's Hospital administered, for the first time in Spain, an experimental gene therapy to a child under the age of three with SPG50, an ultra-rare neurodegenerative disease affecting only around one hundred people worldwide. Prior to the intervention, the hospital conducted a SIMTest—a high-fidelity clinical simulation that made it possible to rehearse every step of the procedure and anticipate potential risks in order to ensure maximum patient safety.
Jordi Clotet, neonatologist at SJD Barcelona Children's Hospital and coordinator of the SIMTest, explains how the simulation was designed, the impact it had on both the team and the procedure, and why this type of preparatory training is transforming the way the hospital approaches its most complex treatments.
How would you define what a SIMTest is, and what would you say are its main objectives?
We define a SIMTest as a high-fidelity clinical simulation used to analyze and improve complex systems or workflows. Unlike other simulations that are primarily training-oriented, in this case the goal is not to practice a specific technique or skill, but rather to realistically reproduce an entire procedure in order to assess how teams, spaces, and resources interact.
The objective is to detect potential risks or difficulties, identify successful practices, and propose improvements that make the process safer for the patient, more efficient for the organization, and more manageable for professionals. Ultimately, a SIMTest allows us to bring together different perspectives on how work is carried out: what is envisioned, what is prescribed, what is communicated or articulated about practice, and what actually happens in reality.
By reproducing a process in a simulated environment, we can identify discrepancies between these perspectives, understand their underlying causes, and refine procedures accordingly—achieving clinical practice that is safer, more consistent, and better aligned with real-world care delivery.
What let to the decision to conduct a SIMTest in the case of gene therapy for hereditary spastic paraplegia type 50 (SPG50)?
It was the first time this gene therapy had been performed in Spain, and the procedure involved highly complex logistics, a pediatric patient, and a biologically hazardous drug. These circumstances made it clear that a full procedural simulation beforehand would be essential to optimize team preparedness, ensure safety, and support coordinated and efficient execution on the day of the actual intervention.
The process entailed several significant organizational and technical challenges: preparation of the drug in the Pharmacy Department within a strictly limited administration window, requiring precise coordination with patient readiness; performance of the procedure in the Imaging Department to allow radiological verification of intrathecal needle placement; the need for general anesthesia and intubation to ensure complete immobility during the technique; and, following administration, the implementation of scheduled postural repositioning with the patient sedated and intubated in the Trendelenburg position.
Taken together, these constraints made a prior simulation indispensable in order to anticipate the coordination, safety, and logistical challenges associated with such a highly complex procedure.
Which teams and professionals took part in the simulation, and how was their involvement coordinated?
The request to conduct the simulation came from the Neurology Department, driven by our institution’s culture, where clinical simulation is regarded as a highly valuable tool for strengthening patient safety and team preparation. Neurology contacted the Clinical Simulation Unit to define how we could support the planning and pre-procedural training. All departments involved in the procedure participated in the SIMTest: Neurology, Anesthesiology, Imaging, Inpatient Care, Pharmacy, and orderlies.
Coordination among teams was both an objective and an outcome of the SIMTest design itself. We applied a methodology inspired by design thinking, structured around phases of needs identification, design, implementation, and impact analysis. This approach makes it possible to address not only technical aspects, but also human, organizational, and safety dimensions—ultimately generating a tangible impact on clinical practice.
How did you ensure that the simulation accurately reflected the real-life situation of such a complex patient and procedure?
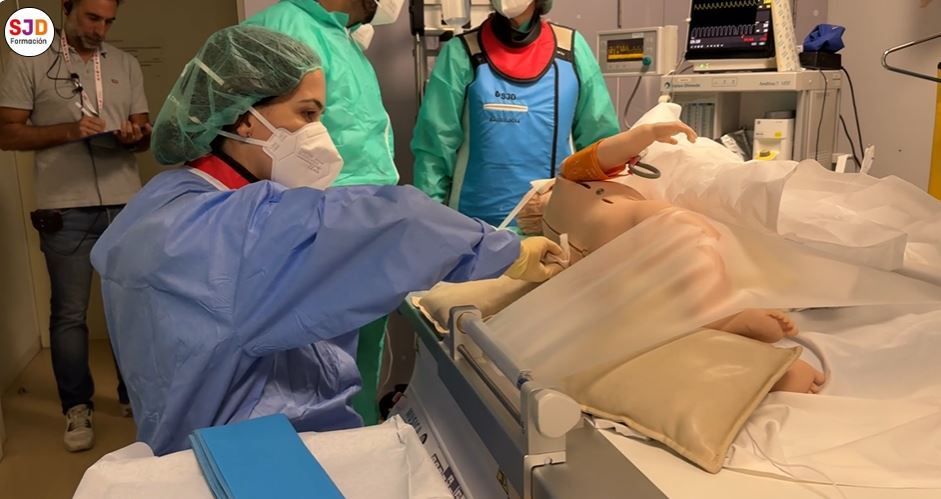
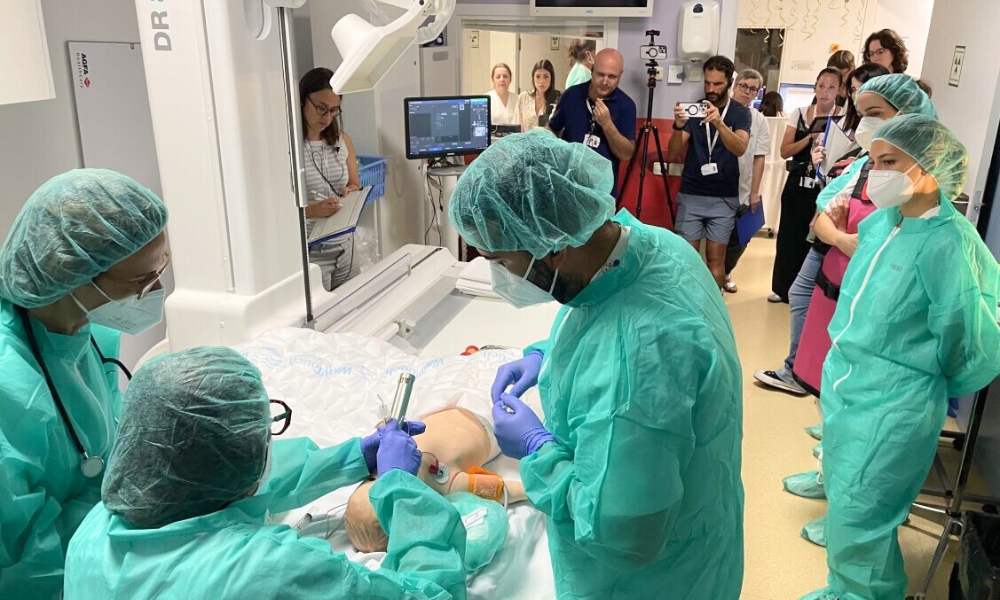
For a simulation to faithfully mirror reality, it is essential to work across different levels of fidelity—not only technical, but also conceptual, environmental, and emotional. In this case, we began with a unified procedural script agreed upon by all the professionals involved, ensuring that every step represented exactly what would be carried out in real clinical practice.
We used the same in-hospital settings—from the inpatient ward to the Imaging suite where the procedure would take place—and the same materials that would be used during the actual intervention: the drug itself, the puncture catheter, and the monitoring devices.
In addition, we used a pediatric manikin adapted with a small fluid reservoir in the lumbar region, which allowed us to realistically recreate the lumbar puncture and the withdrawal of cerebrospinal fluid. This level of preparation created an experience very close to real life, engaging the team both technically and emotionally, and reproducing the degree of concentration, tension, and commitment involved in managing a procedure of such complexity.
How far in advance was the SIMTest planned in relation to the actual intervention, and what factors determined that timing?
The Neurology Department contacted us approximately two months before the procedure was performed on the patient. During that time, we worked on the full design of the SIMTest, defining objectives, scenarios, and coordination among the different teams involved.
The simulation took place one week before the actual procedure. This timing allowed us to thoroughly analyze everything that had occurred, identify areas for improvement, and produce a feedback report outlining the main findings and proposed solutions. This feedback was shared with all participating departments so they could implement the necessary adjustments prior to the real intervention.
What role would you say the simulation played in ensuring procedural safety?
I would say it was a key component. It enabled us to identify potential risks—ranging from communication issues to technical details—and address them before the real procedure took place.
This was a highly complex intervention: the biologically hazardous drug had to be prepared within a maximum four-hour window; the procedure required general anesthesia and intubation in a non-routine setting; and it involved a radiography-guided lumbar puncture followed by postural maneuvers to facilitate proper distribution of the therapy.
The SIMTest made it possible to rehearse team coordination, timing synchronization, drug handling and biosafety measures, as well as the safe mobilization of the patient.
Were there any significant changes to the technique or logistics after rehearsing the procedure?
Following the simulation, we compiled a table with more than 60 observations, documenting both successful adaptations and identified challenges, along with their analysis in terms of causes, effects, and possible solutions. This work enabled us to implement very concrete improvements in the real case.
Team coordination was redefined by appointing a primary point of contact to centralize communication, and the process timeline was adjusted: the patient arrived before the drug, avoiding delays and reducing biological risk. Specific checklists were also developed, along with a visual layout plan for equipment distribution in the room, improving ergonomics and safety.
Biosafety measures were further strengthened—with separate containers for personal protective equipment (PPE) and sharps—and patient positioning was reviewed to ensure more stable fixation during postural changes.
Beyond the technical aspects, the simulation had a highly positive impact on the team, who expressed great satisfaction at having been able to rehearse the procedure. The experience fostered confidence, cohesion, and a shared sense of control—essential elements in such a complex and novel process.
For the family, knowing that the entire procedure had been rehearsed also conveyed a message of trust and commitment. Ultimately, the intervention was carried out successfully and without complications, and part of that outcome can be attributed to the preparatory work conducted through the simulation.
What lessons were learned that can be applied to future interventions involving gene therapies or rare diseases?
This case has demonstrated that the Clinical Simulation Unit is fully integrated into the hospital’s operational framework and is naturally incorporated into the planning of complex procedures, such as gene therapies and rare diseases. The experience confirms that simulation is not a one-off resource, but rather a strategic tool for improving patient care and an essential component of our safety culture.
The commitment to doing things properly—rigorously and collaboratively—is what allows high-realism simulation to have a tangible impact. When this mindset is combined with a structured methodology and in-depth process analysis, the results are remarkable: better-prepared teams, safer procedures, and greater collective confidence when facing unprecedented clinical challenges.
What future do you see for simulation in advanced therapies? Are you preparing other simulations for new treatments or rare diseases?
I believe high-realism simulation will become firmly established as a benchmark tool for addressing procedures that share certain characteristics: high technical complexity, clinical or biological risk, low frequency, or the need to coordinate multiple departments.
The decision to implement a SIMTest should be based on clear criteria—such as the degree of novelty of the procedure, its potential impact on patient safety, the number of departments involved, and the operational cost–benefit balance. When these conditions are met, simulation delivers a clear return: it helps refine processes, reduce risks, and prepare teams under conditions that closely mirror reality.
Each new project generates insights that enrich our practice and further consolidate simulation as an essential component of how we work.
How would you describe the culture of simulation at SJD Barcelona Children's Hospital and its role in the hospital’s future?
At SJD Barcelona Children's Hospital, simulation is embedded in our culture of safety and training. We do not view it solely as a teaching tool, but as a quality-of-care strategy serving continuous improvement.
As a tertiary-level hospital, we manage highly complex pediatric conditions and perform pioneering procedures. In this context, simulation plays a crucial role: it enables us to anticipate clinical scenarios, train multidisciplinary teams, and ensure maximum safety in highly specialized interventions.
An increasing number of departments are incorporating simulation to prepare procedures and optimize processes, reinforcing a culture of excellence that is part of the hospital’s DNA.







